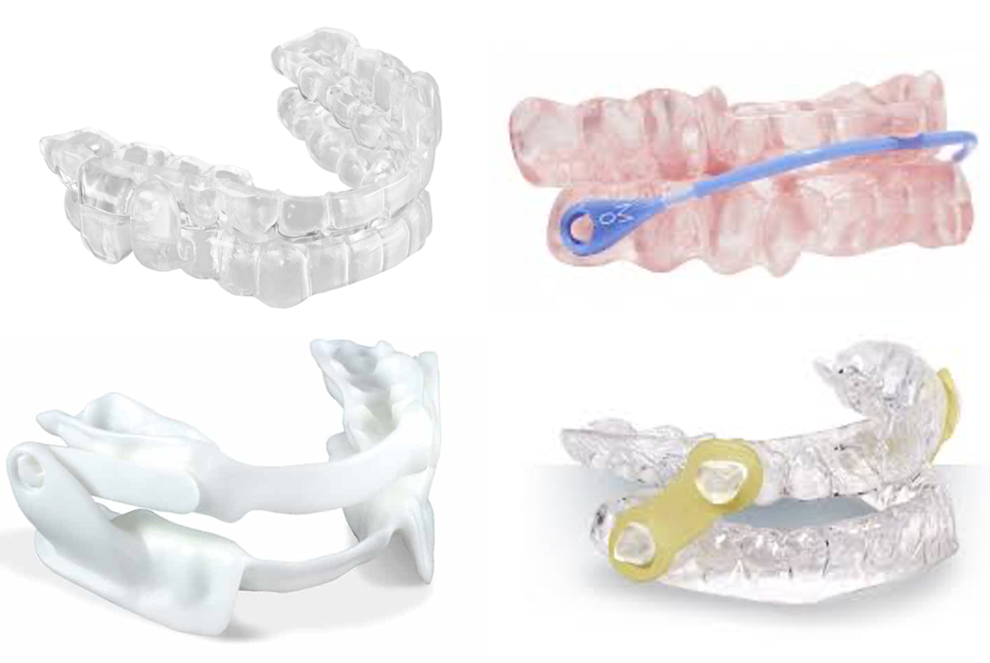
SHOW PATIENTS THE OFF RAMP
Overloading your patient with options is a dental sleep consult equivalent of the Cheesecake Factory menu. Narrow the choices to two or three options and briefly describe how each device’s key features deliver significant benefits. You wouldn’t just open the refrigerator and ask a four-year-old what they want for dinner, right? You ask if they want peas or carrots.
 Robert Cialdini’s “contrast principle” holds that we understand something better when we see it compared to something else. For example, you could juxtapose a bulky OTC appliance with a SomnoDent Avant and a ProSomnus EVO Select. Like Black Sheep said, “You can get with this, or you can get with that…”
Robert Cialdini’s “contrast principle” holds that we understand something better when we see it compared to something else. For example, you could juxtapose a bulky OTC appliance with a SomnoDent Avant and a ProSomnus EVO Select. Like Black Sheep said, “You can get with this, or you can get with that…”
Features are how something works. Benefits are why it matters. Unless your patient is a materials engineer, they’re not going to care about the tensile strength of an appliance’s PMMA trays. Nobody gives a damn about “titratable one-millimeter straps, color-coded for strength and flexibility.”
Features may matter, but only when you connect them to benefits. If you’re still uncertain about how to distinguish a feature from a benefit, ask yourself, so what?
“This one is made from a super strong material.” So what? “Looking at your teeth and your jaw muscles, I can see that you grind your teeth. This Panthera device will withstand all that grinding. It’s the device I wear each night. Only the best for us, right?”
“The EMA bands are easy to swap out, and they come in various different lengths and strengths.” So what? “We can customize the device to your mouth, and if anything changes, we can swap out the straps quickly and easily. That way you won’t have to get a new one prematurely. Good sleep is priceless, but it’s not cheap.”
 SAVE IT FOR THE STUDY CLUB, BUDDY
SAVE IT FOR THE STUDY CLUB, BUDDY
Dentists often assume that patients who’ve been diagnosed and referred have been given thorough explanations about the cause of their sleep apnea, its impacts on their health, and available treatment options. However, an informal survey of patients at one DSM office revealed that more than 90% of patients were virtually uninformed about OSA.
Avoid the study club vernacular. Don’t tell your patient that she has an Apnea Hypopnea Index of 27 and there were associated O2 desats with a nadir of 82 percent.
Think about how you’ve felt in some Embassy Suites conference room for a CE course after the lecturer spent 2 hours on the first slide inundating you with their credentials and the following 6 hours trying to make you think that she, and she alone, is the only person who can operate a successful sleep practice. This information isn’t transmitted to you in a way that’s digestible or actionable. That sucks. Don’t do it to others.
Remember your favorite dental school instructors and most resonant DSM lecturers? They conveyed complex concepts in simple, relatable terms. Jazz musician Charles Mingus once said, “Making the simple complicated is commonplace. Making the complicated simple, awesomely simple, that’s creativity.”
THIS IS WHAT IT SOUNDS LIKE…SO WHAT?
Consider this example from a sleep coordinator explaining test results in understandable terms. “Ms. Jackson, it looks like you stop breathing 27 times per hour while you’re asleep. During that time, your brain isn’t getting the oxygen it needs; your heart is racing because your body is suffocating. This happens over and over again, all night long.”
Then she pauses to connect the dots and answer the unspoken “so what?”
 The sleep coordinator continues: “When your heart is racing like this, 27 times per hour, more than 200 times per night, it’s overworking all night, leading to a 140 percent increased risk of heart attack and double the risk of stroke. Each time you stop breathing, your brain forces you to wake up, not all the way, but enough. That’s why you’re tired all the time. I’m sure you can see how important it is that we do everything we can to take care of this, Ms. Jackson.”
The sleep coordinator continues: “When your heart is racing like this, 27 times per hour, more than 200 times per night, it’s overworking all night, leading to a 140 percent increased risk of heart attack and double the risk of stroke. Each time you stop breathing, your brain forces you to wake up, not all the way, but enough. That’s why you’re tired all the time. I’m sure you can see how important it is that we do everything we can to take care of this, Ms. Jackson.”
Note how the sleep coordinator artfully explained a complex and serious health matter in plain language, emphasized how dangerous it can be, cited a couple meaningful statistics, and closed by tying it to the patient’s chief complaint: excessive sleepiness during the day. Finally, the sleep coordinator drove home the fact that they can likely help her.
You can flaunt your encyclopedic OAT knowledge at conferences, but you need a whole different style when advising a patient. Limit the options to around three viable solutions and then tie the features to impactful benefits. Then …
ALWAYS BE CLOSING
We asked, So what?
Time to ask, Now what?
You’re not doing this for your health; you’re doing it for theirs. This exchange of information is pointless if we don’t prompt them to act after you explain their options.
 Give your patient an off-ramp to make the sensible decision. “Which device would you like to take impressions for today?”
Give your patient an off-ramp to make the sensible decision. “Which device would you like to take impressions for today?”
Give your physician counterpart an off-ramp by asking how she’d like you to refer patients and who on her end should receive your referral forms so she can do the same for you.
Actively listen and stay attuned to nonverbal cues. If you sense reluctance, it’s not the end of the world. Say, “It’s important for you to have all the information you need. What questions do you have?” Listen and give active feedback (“So what I hear you saying is …”). Clarify their questions and address their lingering concerns. Speak with accuracy and precision.
Show them the off-ramp and they’ll show you the money.
————————————————————————————————————————————————————————————————————–
If you have a 100% consultation-to-treatment conversion rate, more physician referrals than you know what to do with, and have all the most updated information on medical billing, appliance design, sleep marketing, and everything else Dental Sleep Medicine related, then you shouldn’t come to the 2024 Transform Dental Sleep Symposium.
For everyone else that is committed to continually improving your Dental Sleep Practice, learning from the best in the field, and having a lot of fun while doing it, you should absolutely register yourselves and your team for the Transform Dental Sleep Symposium in Scottsdale, AZ on February 2-3, 2024.

Stay informed about Jason’s books, media, & adventures
SUBSCRIBE FOR MORE INFO


GUEST POST BY DR. JEFF RODGERS: IF YOU DON’T LIKE YOUR LIFE, CHANGE IT

